Our Services
Skin Rashes and Disorders
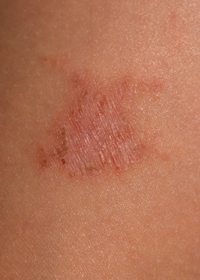 Rashes are changes in the skin's color or texture. Simple rashes are called dermatitis, which means the skin is inflamed or swollen. Some rashes are independent symptoms, but many cause itching, burning or other discomfort. There are a great many reasons for individuals to develop rashes.
Rashes are changes in the skin's color or texture. Simple rashes are called dermatitis, which means the skin is inflamed or swollen. Some rashes are independent symptoms, but many cause itching, burning or other discomfort. There are a great many reasons for individuals to develop rashes.
Types of Rashes
Rashes occur for a variety of reasons, some relatively benign, some extremely serious. Many rashes look similar to one another so their causes may be difficult to diagnose.
Contact Dermatitis
Contact dermatitis is caused by an irritating substance. In some cases, the substance is universally irritating, like certain chemicals. In others, the irritation is the result of an allergen, such as latex, perfume, dye, or animal dander, that irritates only individuals with particular sensitivities. Plants like poison ivy and insect bites cause rashes in some individuals.
Allergic Rashes
Apart from contact dermatitis, patients may develop allergic rashes as a reaction to ingested allergens. Certain food stuffs and medications can trigger hives or other rashes in sensitive individuals.
Seborrheic Dermatitis
Seborrheic dermatitis occurs when the skin forms red, scaly, flaking patches. Though most common on the face and on the head, where it is known as dandruff or cradle cap, the condition can also be evident in the outer ear, on the eyebrows or eyelashes, forehead, sides of the nose, or chest and upper back.
Viral or Bacterial Skin Conditions
Other skin conditions, like eczema, psoriasis, impetigo, or pityriasis rosea, frequently cause rashes. Each may be diagnosed by its pattern, whether the rash is flat or pustular, and on what part of the body it occurs, although distinguishing the rashes may at times be difficult.
Systemic Diseases
Many systemic diseases have rashes as one of their symptoms. These include disorders often characterized as childhood diseases, like measles, chicken pox, rubella and scarlet fever, shingles, a disease caused by the same virus that is responsible for chicken pox, autoimmune diseases such as rheumatoid arthritis and lupus, and some sexually transmitted diseases, such as syphilis.
Rashes Caused by Sun or Heat
Heat rash is a common ailment in infants, but can occur in individuals of any age, causing small red spots or bumps which may be itchy. This rash develops when the sweat ducts in the skin are clogged, interfering with the normal process of perspiration. Too much exposure to the sun to the ultraviolet light of tanning salons may also cause a rash on affected areas. This type of rash is sometimes referred to as "sun poisoning" but the scientific name for it is polymorphous light eruption or PMLE.
Stress Rashes
Under certain circumstances, some individuals may develop rashes from stress alone, without another precipitating cause.
Treatment of Rashes
When a rash is caused by an underlying condition or disease process, the patient must be treated for the pervasive disorder. When a rash is the result of a bacterial infection, it is treated with antibiotics. When a rash stems from a virus, it may be treated with antiviral medication. Allergic rashes are normally treated with antihistamines and, when more severe, with corticosteroids. In many cases, avoidance of contact with the irritating substance or material may be sufficient to help the rash abate.
Almost all rashes that cause itching can be treated symptomatically with one or more of the following: antihistamines, soothing lotions like Calamine, topical or oral corticosteroids, baths with colloidal oatmeal, moisturizing creams or cold compresses. Wearing soft, loose clothing and taking over-the-counter pain relievers may also provide relief.
Sports Related Injuries
 Special treatment is often needed for athletes who overuse their feet and ankles. Our sports and dance medicine specialty provides support for conditions such as stress fractures, heel pain, Achilles tendonitis and neuromas. Whether you are a professional, amateur or recreational athlete, you are often at risk for foot problems.
Special treatment is often needed for athletes who overuse their feet and ankles. Our sports and dance medicine specialty provides support for conditions such as stress fractures, heel pain, Achilles tendonitis and neuromas. Whether you are a professional, amateur or recreational athlete, you are often at risk for foot problems.
Sports-related conditions can occur as a result of injury, wear-and-tear or infection. Different activities place different areas at a higher risk for damage, so it is important to take the necessary precautions to protect your feet. Treatment for sports-related conditions can involve surgery, orthotics, physical therapy and rest.
While treatment varies depending on the type and severity of the condition, our doctors are experienced in working with athletes of every kind to help them recover as quickly and effectively as possible in order to return to their chosen sport.
Sprains and Strains
A sprain involves a tearing a ligaments as a result of a sports injury, fall, accident or other type of trauma. Sprains of the foot usually occur within the midfoot or the base of the big toe, a condition known as turf toe. Midfoot sprains often occur by twisting the foot in an odd way, while toe sprains are usually caused by hyperextension of the big toe.
Patients with a foot sprain may experience swelling, tenderness, bruising and pain in the affected area. Bearing weight on the foot may be difficult for some patients as well. Your doctor can diagnose a sprain after performing a physical examination of the foot and asking you questions about your symptoms and the injury. X-ray images may also be taken to confirm the diagnosis.
Foot sprains can usually be treated through conservative methods such as resting the foot, applying ice, wearing compression bandages and keeping the foot elevated. Your doctor may also prescribe medication or recommend anti-inflammatory drugs to help reduce pain and swelling. Severe sprains may require immobilizing the foot in a cast and avoiding walking for some time. Most sprains do not require surgery, and patients will be able to resume physical activity once the injury heals.
Tendon Repair
 Tendon repair is a surgical procedure used to repair torn or damaged tendons for patients experiencing pain, swelling and limited function. Tendons are the cord-like structures made of fibrous tissue that help connect muscles to bones. Tendon injuries are common, and most frequently occur in the shoulder, elbow, knee and ankle joints.
Tendon repair is a surgical procedure used to repair torn or damaged tendons for patients experiencing pain, swelling and limited function. Tendons are the cord-like structures made of fibrous tissue that help connect muscles to bones. Tendon injuries are common, and most frequently occur in the shoulder, elbow, knee and ankle joints.
The tendon repair procedure can be performed under local or general anesthesia on an outpatient basis. During the procedure, the torn ends of the tendon are sewn back together to relieve pain and restore function to the affected area. If the tendon has been severely damaged, a tendon graft may be needed, which is usually taken from the patient's foot or toe.
After the procedure, the treated area will be kept in a splint or cast for several weeks. Full healing usually takes six to 12 weeks, after which patients can enjoy full joint use once again.
While this procedure is considered safe for most patients, there are certain risks associated with any surgical procedure, including infection, bleeding, formation of scar tissue and partial loss of use within the affected joint. These risks are considered rare, with most patients achieving successful results from the tendon repair procedure.
